Introduction
You went and got the MRI. Maybe your doctor ordered it, maybe you pushed for it yourself. Either way, the report comes back and suddenly you’re staring at words like “disc degeneration,” “disc bulge,” and “facet arthropathy.” It sounds like your spine is falling apart.
Take a breath.
As a team of physiotherapists, chiropractors, and strength coaches who work with people in pain every single day, we can tell you this with confidence: disc degeneration is overwhelmingly normal. It happens to virtually everyone as they age, and in most cases, it is not the reason you’re in pain.
This blog will walk you through the research—including a landmark study that scanned thousands of people without back pain—to show you just how common these findings are. More importantly, we’ll talk about what actually matters when it comes to managing back pain.
Dealing with back pain and not sure where to start? Book an assessment with our team at Vital Performance Care. We’ll cut through the noise, look at the full picture, and build a plan that actually gets you moving. Book here.
What Is Disc Degeneration?
Your spine is made up of vertebrae stacked on top of each other, with intervertebral discs sitting between them. These discs act as shock absorbers—they help distribute load, allow movement, and provide cushioning. They’re made of a tough outer ring (the annulus fibrosus) and a gel-like centre (the nucleus pulposus).
Over time, these discs lose hydration, become less flexible, and may show changes on imaging. This is what’s referred to as “disc degeneration” or “degenerative disc disease”—though calling it a “disease” is misleading. It’s not a disease at all. It’s a natural process, much like getting grey hair or developing wrinkles. It happens to everyone.
The kicker? Most people with disc degeneration have zero symptoms. The degeneration is there on the MRI, but they’re walking, running, lifting, and living their lives without any issues. This is one of the most important and misunderstood facts in musculoskeletal health.
The Brinjikji Study: Degeneration Is Normal
If there’s one study that every person with back pain should know about, it’s the 2015 systematic review by Brinjikji et al., published in the American Journal of Neuroradiology. The researchers reviewed 33 studies involving over 3,100 asymptomatic individuals—people with no back pain whatsoever—and looked at what their MRIs showed.
The results were striking:
- At age 20, 37% of pain-free individuals already showed disc degeneration on MRI.
- By age 50, that number jumps to 80%.
- By age 80, 96% of pain-free people had disc degeneration.
- Disc bulges were present in 30% of 20-year-olds and 84% of 80-year-olds – again, all without symptoms.
- Even disc protrusions were found in 29% of 20-year-olds with no pain.
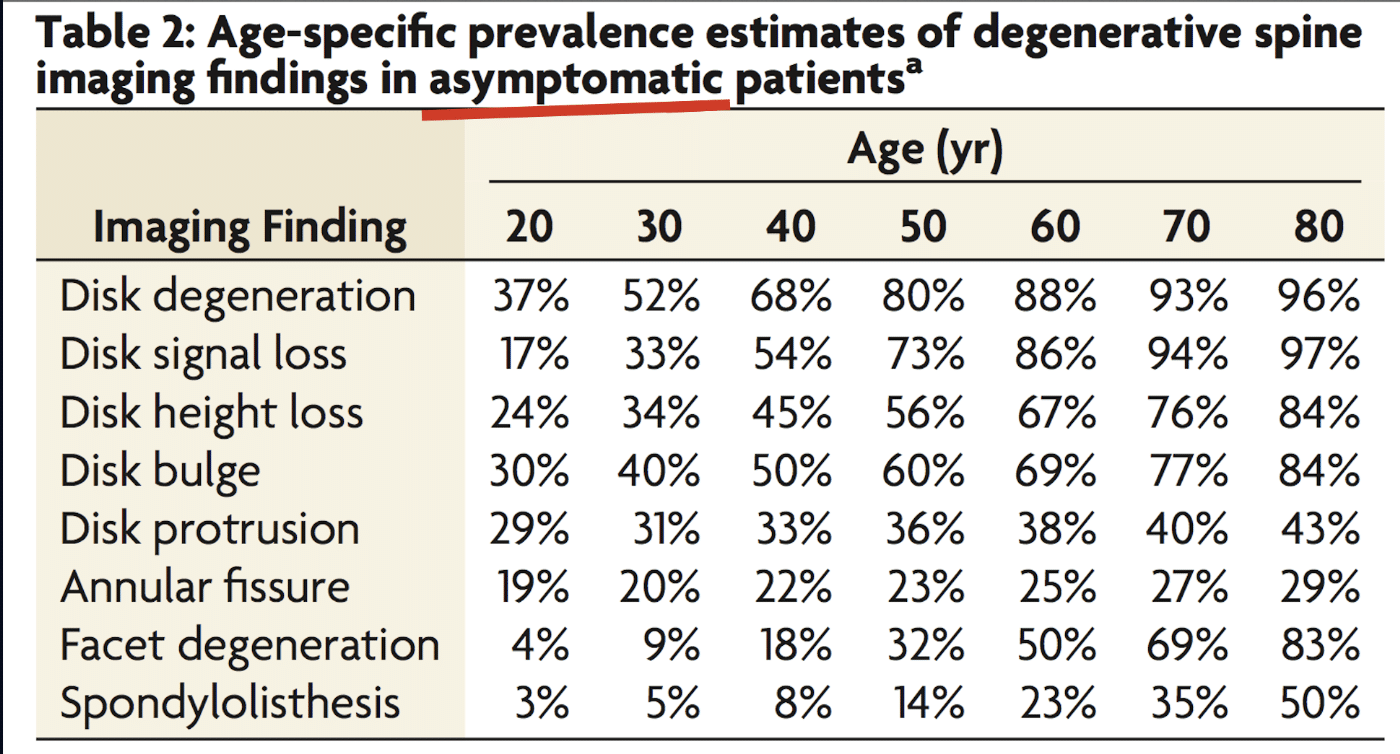
Brinjikji et al 2015 Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. AJNR Am J Neuroradiol. 2015 Apr;36(4):811-6.
Read that again: the vast majority of people walking around pain-free have “abnormalities” on their MRIs. These findings are so common that calling them “abnormal” is a bit like calling grey hair a medical condition. Imaging does not always correlate to function, and it certainly doesn’t tell the whole story.
Why Your MRI Report Sounds Scary (But Shouldn’t Be)
MRI reports are written by radiologists, and their job is to document everything they see. The language they use – “degenerative changes,” “disc desiccation,” “moderate central canal stenosis” – is clinical and precise. But it’s not designed to be read by the average person. Without context, it can sound terrifying.
Here’s the problem: when someone in pain reads their MRI report and sees “disc degeneration at L4-L5,” they understandably connect the dots. “I’m in pain. The MRI found something. That must be the cause.”
But as we’ve seen from the Brinjikji data, those same findings exist in millions of people who feel perfectly fine. The imaging finding doesn’t automatically equal your pain generator. This is why at Vital Performance Care, we always tell people: before you rush to get that MRI, ask yourself – would it change what you do?
In many cases, the answer is no. The treatment plan – progressive loading, movement modification, strengthening – remains the same whether or not you have imaging. And in some cases, the MRI can actually do more harm than good by creating fear and avoidance behaviours around movement.
What Actually Matters for Back Pain
If disc degeneration isn’t the villain, what is? Back pain is complex and multifactorial. Here are the things that actually influence your experience of pain:
Load Management
Just like running injuries come from doing too much too fast, back pain often comes from a mismatch between what you’re asking your body to do and what it’s prepared for. A sudden spike in activity – whether that’s a heavy deadlift, a long drive, or a weekend of yard work – can overload tissues that weren’t ready. The fix isn’t rest. It’s building capacity gradually.
Sleep, Stress, and Recovery
Pain is processed by the nervous system, and your nervous system is influenced by far more than just what’s happening in your spine. Poor sleep, high stress, anxiety, and low mood all amplify pain sensitivity. Addressing these factors is often just as important as the physical rehab.
Strength and Movement Quality
Weak or poorly coordinated muscles around the hips, core, and spine can contribute to recurring back pain. The research consistently shows that exercise is one of the most effective treatments for low back pain—and not just any exercise, but targeted, progressive loading that builds real capacity. We use tools like force plates and dynamometers at Vital to objectively measure where the gaps are and track your progress.
What that strengthening looks like also depends on where and how the degeneration is affecting you functionally. For example, if the degeneration is at the facet joint and you report pain when extending your low back, we’re not going to load you into more extension. Instead, we might prioritize strengthening the anterior chain, incorporate more low back flexion-based mobility and stability work, and focus on glute and hip dissociation—teaching your body to use the other muscles in your posterior chain rather than defaulting to low back extension every time. It’s not about avoiding movement. It’s about choosing the right movements for where you’re at right now and building from there.
Regenerative Injections
For some people, targeted regenerative injections can play a meaningful role alongside rehab. Options like PRP (platelet-rich plasma), prolotherapy, Durolane, and other regenerative treatments can help manage pain, support tissue healing, and potentially slow further breakdown — especially when combined with the right loading and strengthening program. At Vital Performance Care, we have a sport medicine doctor on our team who does consultations covered by Alberta Health, so there’s no barrier to finding out whether these options make sense for you. If you’re curious, email or call us to book a consultation and we’ll point you in the right direction.
Beliefs and Expectations
This might sound surprising, but what you believe about your pain matters enormously. If you’ve been told your spine is “degenerating” and you should “avoid bending,” you’re likely to move less, fear activity, and ultimately get weaker—which feeds the pain cycle. Reframing how you think about your spine is a powerful part of recovery. Your spine is strong. It’s designed to move, bend, lift, and twist. Degeneration doesn’t change that.
What We Do at Vital Performance Care
At Vital Performance Care in Calgary, we take a comprehensive, evidence-based approach to back pain. We don’t just look at your MRI and call it a day—we look at the full picture: how you move, how strong you are, what your day-to-day demands look like, and what’s going on in your life that might be contributing. The truth is, there could be a lot of different things contributing:
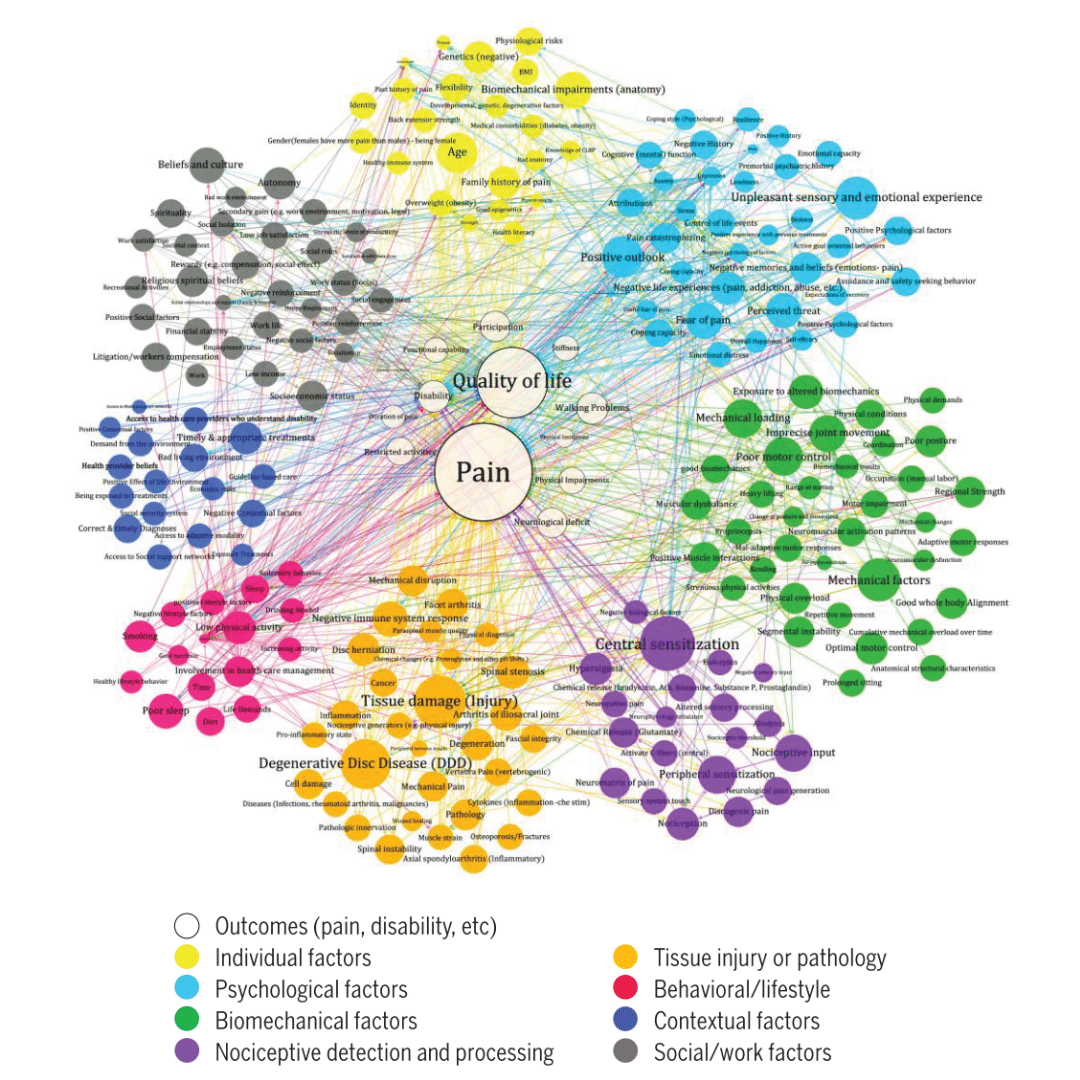
Our team includes physiotherapists, chiropractors, and strength coaches who work collaboratively to build you a plan that actually gets results. We’re equipped with force plates, dynamometers, shockwave therapy, dry needling, blood flow restriction training, and more—because the right tools, combined with the right plan, make a real difference.
Whether you’re dealing with your first episode of low back pain or you’ve been battling it for years, we’re here to help you move better, feel stronger, and stop worrying about what your MRI says.
Conclusion
Disc degeneration is not a death sentence for your spine. It’s a normal part of aging that the overwhelming majority of people experience—most without any pain at all. The Brinjikji et al. (2015) study made this crystal clear: imaging findings like disc degeneration, disc bulges, and even disc protrusions are incredibly common in people with zero symptoms.
If you’re in pain, the answer usually isn’t in the MRI. It’s in understanding your body, building strength, managing load, and working with professionals who look beyond the scan.
Ready to take the next step? Book an assessment with our team at Vital Performance Care. We’ll help you understand your pain, build a plan, and get you back to doing what you love. Book an assessment with one of our chiropractors, physiotherapists, or osteopaths to start.
References
Brinjikji, W., Luetmer, P. H., Comstock, B., Bresnahan, B. W., Chen, L. E., Deyo, R. A., Halabi, S., Turner, J. A., Avins, A. L., James, K., Wald, J. T., Kallmes, D. F., & Jarvik, J. G. (2015). Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. American Journal of Neuroradiology, 36(4), 811–816. https://doi.org/10.3174/ajnr.A4173
Chou, R., Fu, R., Carrino, J. A., & Deyo, R. A. (2009). Imaging strategies for low-back pain: Systematic review and meta-analysis. The Lancet, 373(9662), 463–472. https://doi.org/10.1016/S0140-6736(09)60172-0
Hartvigsen, J., Hancock, M. J., Kongsted, A., Louw, Q., Ferreira, M. L., Genevay, S., Hoy, D., Karppinen, J., Pransky, G., Sieper, J., Smeets, R. J., & Underwood, M. (2018). What low back pain is and why we need to pay attention. The Lancet, 391(10137), 2356–2367. https://doi.org/10.1016/S0140-6736(18)30480-X
Steffens, D., Maher, C. G., Pereira, L. S. M., Stevens, M. L., Oliveira, V. C., Chapple, M., Teixeira-Salmela, L. F., & Hancock, M. J. (2016). Prevention of low back pain: A systematic review and meta-analysis. JAMA Internal Medicine, 176(2), 199–208. https://doi.org/10.1001/jamainternmed.2015.7431
Nakashima, H., Yukawa, Y., Suda, K., Yamagata, M., Miyazaki, T., & Abe, T. (2015). Abnormal findings on magnetic resonance images of the cervical spines in 1211 asymptomatic subjects. Spine, 40(6), 392–398. https://doi.org/10.1097/BRS.0000000000000775

More About The Author
Carla Robbins, Co-Founder of Vital Performance Care
Carla’s journey into the world of endurance training, strength and conditioning, and exercise physiology began with her Undergraduate Degree in Exercise Physiology at the University of Calgary and continued into her graduation with a Master’s in Exercise Physiology in 2016. Between working for the Canadian Sports Institute to the creation of her company Vital Strength and Physiology Inc (now Vital Performance Care), Carla is driven by a desire to find better ways to address complex cases in professional and everyday athletes and individuals.



