If you’ve been told to stop deadlifting after a disc herniation – or if your first instinct after a diagnosis was to avoid the gym entirely – you’re far from alone. For decades, the advice was simple: an injured back means no lifting, rest until healed, and treat the spine as fragile. Take a breath. The research tells a more nuanced story. A growing body of evidence suggests that not only can many people with disc herniations safely return to deadlifting, but that appropriately loaded hip-hinge movements may actually support recovery while they strengthen the muscles around the injury. At the same time, technique matters: poor mechanics and excessive spinal flexion under load are genuine risk factors that warrant attention. This blog will walk you through the key concepts – how disc herniations actually happen, why pain doesn’t always mean damage, and a practical exercise progression to help you get back to deadlifting safely.
Not sure where to start? Book an assessment with our team at Vital Performance Care. We’ll look at the full picture and build a plan that gets you moving. Book here.
Most Common Mechanisms
So how do disc herniations actually happen? It’s usually not one dramatic moment. Most of the time, it’s a combination of factors building up over time. Research shows that flexion under compressive load – rounding the lower back while it’s being loaded – is the primary mechanism. When the lumbar spine flexes under load, the gel-like centre of the disc gets pushed toward the back wall, increasing pressure on the outer layers. Over many repetitions, tiny cracks can develop and eventually allow herniation. The most injurious pattern combines flexion (forward bending) with rotation (twisting) and compression (load) all at once. Think: picking something up off the floor while twisting to hand it to someone. Equally important is surprise loading – unexpected forces applied to the spine before your muscles have time to brace. This is why back injuries often happen during mundane activities like picking up a light object, not necessarily during heavy barbell work where the muscles are already engaged. The key takeaway is that t’s rarely one big event. It’s usually cumulative stress, poor positioning, and lack of preparedness – all of which are things you can address.
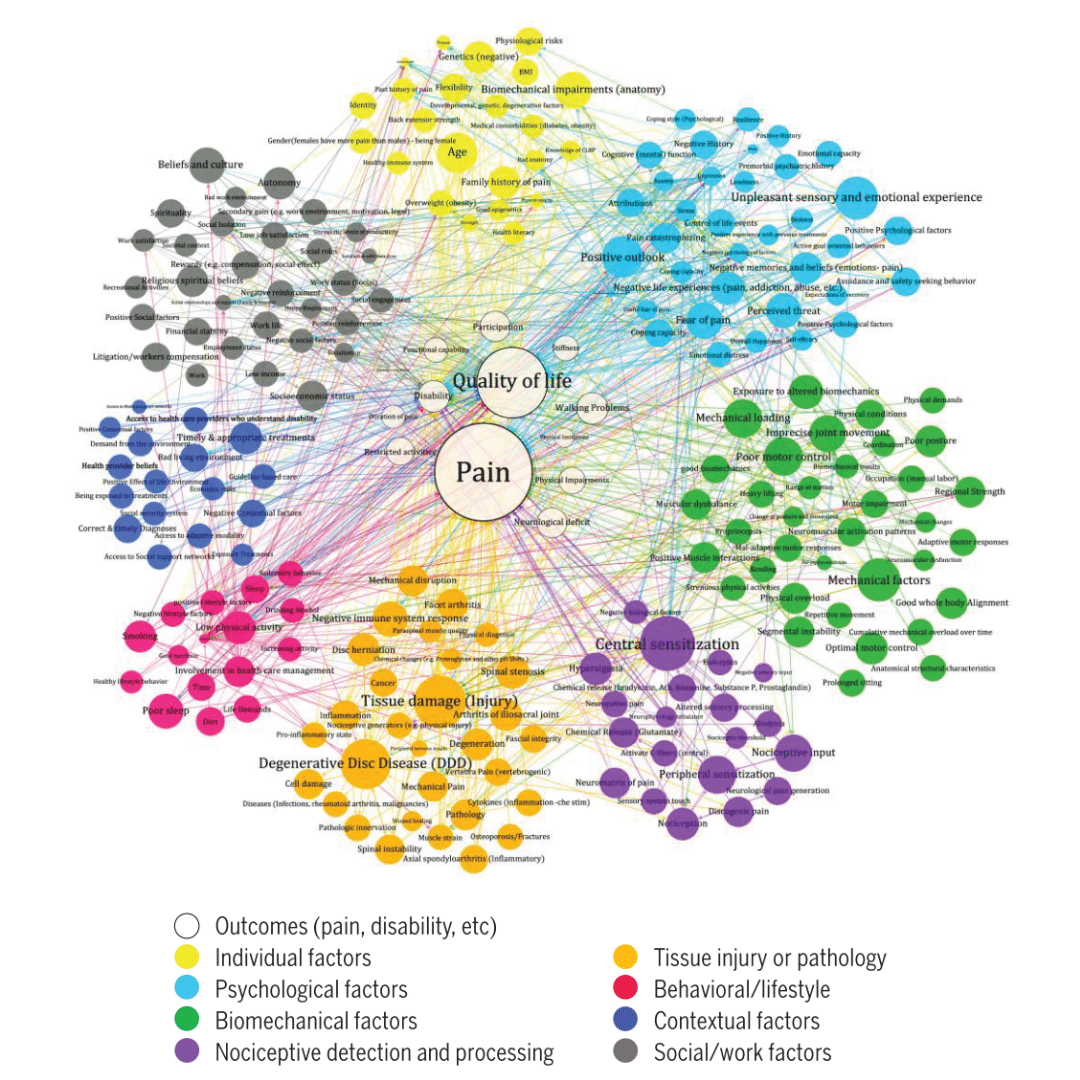
Figure: The pain web — a network of biological, psychological, and social factors that interact to influence pain experience and recovery. [Source: Adapted from Carr & Bradshaw, 2014 / biopsychosocial pain model literature]
Pain Doesn’t Mean Injury
This is one of the most important things to understand: pain and tissue damage don’t always go together. You can have significant findings on an MRI and feel perfectly fine. You can also be in a lot of pain with a scan that looks completely normal. The landmark study by Brinjikji et al. (2015) showed this clearly. The researchers reviewed MRIs of over 3,100 people with no back pain at all and found that disc herniations, bulges, and degeneration were incredibly common:
- At age 20, 29% of pain-free people already had disc protrusions on MRI.
- By age 50, 80% of pain-free individuals showed disc degeneration.
- Disc bulges were present in 30% of 20-year-olds and 84% of 80-year-olds – all without symptoms.
- Most disc herniations resolve on their own within 12–18 months.
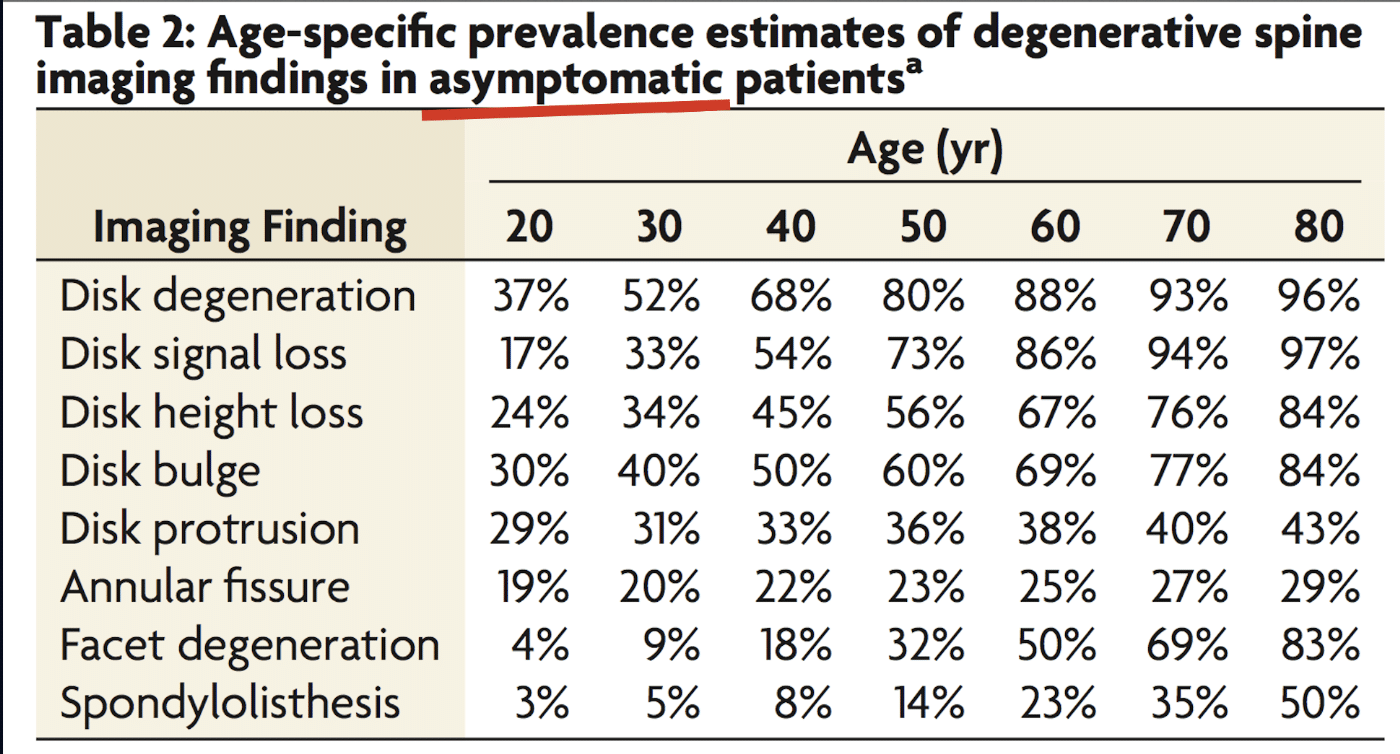
The point is this: a herniation on your MRI doesn’t mean you’re broken, and it definitely doesn’t mean you can’t deadlift. Many people are walking around, training, and living full lives with disc findings they don’t even know about. The old approach – rest, avoid movement, protect the spine – often makes things worse. When pain leads to fear, fear leads to avoidance, and avoidance leads to deconditioning and more pain. The research consistently shows that people who stay active and gradually reload have better outcomes than those who rest and avoid.
Getting Back to Deadlifting: Exercise Progressions
So how do you actually get back to it? The answer isn’t jumping straight to a barbell off the floor. It’s a gradual progression that builds capacity, confidence, and technique step by step.
Here’s a simplified version of how we approach this at Vital Performance Care:
Phase 1: Calm Things Down & Build a Base
The first step is education and gentle movement. Understanding that pain doesn’t equal damage goes a long way. We start with low-load exercises that restore motor control – how your spine, pelvis, and hips coordinate together.
- Bird-dogs – start by dissociating the arms and legs from a neutral spine without too much core bracing needed
- Quadruped Rockback – start patterning a hip squat/hinge without axial load
- Dead bugs like Regular Deadbugs, Wall Deadbugs, Foam Roller Deadbugs
- Glute bridge variations and progressing to SL Glute Bridges
- Gentle spinal mobility: like the quadruped spinal CARs
Phase 2: Introduce the Hip Hinge
The hip hinge – pushing your hips back and bending at the waist while keeping a neutral spine – is the fundamental movement pattern of a deadlift. But it’s also the natural mechanics of every time you pick something up off the floor, load groceries into a car, or grab something from a low shelf. Avoiding it doesn’t protect your spine. It deconditions it.
- Bodyweight hip hinges with a dowel – learn the hinge pattern first – you use this in activities of daily living so it’s good to practice!
- Staggered Stance Hinges
- Hinges with different implements and pressures, like the foam roller hinge or knee-supported hinge
- Hinges with dumbbells
- Trap bar deadlifts – these keep the load closer to your center of mass, reducing demand on the lower back while still training the posterior chain. Think of it as a “squatty deadlift”
Phase 3: Progressive Loading
Once you’re moving well and pain-free with lighter loads, it’s time to gradually increase. This is where we use objective tools like force plates and dynamometers at Vital to track your progress and make sure you’re building real strength.
- RDL’s with dumbbells or barbells
- Conventional or sumo deadlifts (based on your anatomy and comfort)
- Hip thrusts, Single Leg Hip Thrusts, and Staggered Hip Thrusts
- 45 degree back extensions with glute focus, single leg back extensions, and eventually even GHR back extensions.
A note on pain during training: Pain at or below 5/10 during exercise is generally considered tolerable and does not indicate tissue damage. If pain returns to baseline within 24 hours, the load was appropriate. Pain above 5/10 or that lingers into the next day means you should dial it back. The goal is progressive, systematic capacity-building – not pushing through pain.
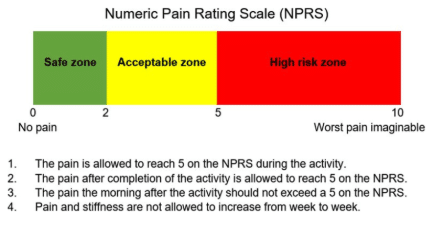
Figure: The Numeric Pain Rating Scale (NPRS) used to guide loading in rehabilitation. A pain level of 0–5 during exercise is generally considered tolerable and acceptable; above 5 warrants load reduction or modification.
Why Form Matters
The research is clear: lifting with poor form – particularly allowing excessive spinal flexion (rounding) during the pull – increases the risk of disc loading patterns associated with injury. A safe deadlift generally involves a neutral lumbar spine, a braced core, bar proximity to the body, and leading with the hips rather than squatting the weight up. But here’s the important part: good technique is not just a matter of watching a YouTube video and copying it. Your body adapts, compensates, and develops habits over years. Someone returning to deadlifting after a herniation may have altered movement patterns and compensations they’re not even aware of. This is why we believe strongly at Vital Performance Care that returning to deadlifting after a back injury should be supervised by a trained professional. An experienced eye can identify form breakdowns that a mirror cannot, and a progressive program can be tailored to your specific anatomy, injury history, and movement patterns.
Real-World Example: Nicholas Simpson – one of Vital Performance Care’s associates, has suffered multiple disc herniations over the years, and despite MRI’s confirming they are still there, he has rehabbed them to the point of no pain and ability to lift and run normally again. His personal experiences plus his deep knowledge on injuries and rehabilitation make him a great choice for a trainer if you’re in need of one!

What We Do at Vital Performance Care
At Vital Performance Care in Calgary, we take a comprehensive, evidence-based approach to getting you back to deadlifting. We don’t just look at your MRI – we look at the full picture: how you move, how strong you are, what your day-to-day demands look like, and what’s going on in your life that might be contributing. Our team includes physiotherapists, chiropractors, and strength coaches who work collaboratively to build you a plan that actually gets results. We’re equipped with force plates, dynamometers, shockwave therapy, dry needling, blood flow restriction training, and more – because the right tools, combined with the right plan, make a real difference.
Conclusion
A disc herniation is not a death sentence for your deadlift. The research shows that most herniations resolve on their own, that imaging findings don’t always correlate with pain, and that progressive loading – done with good technique and professional guidance – is one of the best things you can do for your spine. The hip hinge is a fundamental human movement. Avoiding it entirely doesn’t protect the spine – it deconditions it. With the right approach – starting where you are, building gradually, and working with professionals who understand the nuance – you can get back to deadlifting and feel stronger than before. Ready to take the next step? Book an assessment with our team at Vital Performance Care. We’ll help you understand your pain, build a plan, and get you back to doing what you love. Book your assessment here.
References
Aasa, B., Berglund, L., Michaelson, P., & Aasa, U. (2015). Individualized low-load motor control exercises and education versus a high-load lifting exercise and education to improve activity, pain intensity, and physical performance in patients with low back pain: a randomized controlled trial. Journal of Orthopaedic & Sports Physical Therapy, 45(2), 77–85.
Adams, M. A., & Hutton, W. C. (1982). Prolapsed intervertebral disc: a hyperflexion injury. Spine, 7(3), 184–191.
Autio, R. A., Karppinen, J., Niinimäki, J., Ojala, R., Kurunlahti, M., Haapea, M., & Tervonen, O. (2006). Determinants of spontaneous resorption of intervertebral disc herniations. Spine, 31(11), 1247–1252.
Berglund, L., Aasa, B., Hellqvist, J., Michaelson, P., & Aasa, U. (2015). Which patients with low back pain benefit from deadlift training? Journal of Strength and Conditioning Research, 29(7), 1803–1811.
Brinjikji, W., Luetmer, P. H., Comstock, B., et al. (2015). Systematic literature review of imaging features of spinal degeneration in asymptomatic populations. American Journal of Neuroradiology, 36(4), 811–816. Camara, K. D.,
Coburn, J. W., Dunnick, D. D., Brown, L. E., Galpin, A. J., & Costa, P. B. (2016). An examination of muscle activation and power characteristics while performing the deadlift exercise with straight and hexagonal barbells. Journal of Strength and Conditioning Research, 30(5), 1183–1188.
Carroll, B., & McGill, S. (2018). Gift of Injury: The Strength Athlete’s Guide to Recovering from Back Injury and Winning Again. BackFitPro Inc. Chiu, C. C., et al. (2015). The probability of spontaneous regression of lumbar herniated disc: a systematic review. Clinical Rehabilitation, 29(2), 184–195.
Cholewicki, J., McGill, S. M., & Norman, R. W. (1991). Lumbar spine loads during the lifting of extremely heavy weights. Medicine and Science in Sports and Exercise, 23(10), 1179–1186.
Hales, M. E., Johnson, B. F., & Johnson, J. T. (2009). Kinematic analysis of the powerlifting style squat and the conventional deadlift during competition. Journal of Strength and Conditioning Research, 23(9), 2574–2580.
McGill, S. M. (2007). Low Back Disorders: Evidence-Based Prevention and Rehabilitation (2nd ed.). Human Kinetics.
Videman, T., Battié, M. C., Gibbons, L. E., Gill, K., Fisher, L. D., & Manninen, H. (1997). Lifetime exercise and disk degeneration: an MRI study of monozygotic twins. Medicine and Science in Sports and Exercise, 29(10), 1350–1356.

More About The Author
Carla Robbins, Co-Founder of Vital Performance Care
Carla’s journey into the world of endurance training, strength and conditioning, and exercise physiology began with her Undergraduate Degree in Exercise Physiology at the University of Calgary and continued into her graduation with a Master’s in Exercise Physiology in 2016. Between working for the Canadian Sports Institute to the creation of her company Vital Strength and Physiology Inc (now Vital Performance Care), Carla is driven by a desire to find better ways to address complex cases in professional and everyday athletes and individuals.